We have endured another round of Industrial Action this month and yet again, we have seen many staff working differently, doing things they would not normally do and stepping into different environments and departments. This has been an incredibly challenging time, but I continue to be amazed by the resilience, flexibility and team work of all of our staff, and I would like to say a big thank you again to everyone for all that you continue to do.
The indicative ballot for Speciality and Specialist doctors has just closed, but there are no further strike dates in the diary at present so we do at least have a little reprieve this month.
This month, I thought it would be good to look up from immediate pressures and to focus on some of the many great things we can celebrate and be proud of.
Research and Evaluation update
Within Norfolk and Waveney ICB we have an amazing research and innovation team. Their role is to expand the reach and impact of research across our community. They work to build our research capacity, to support people with good ideas but little experience of research, and to entice new people to start research, working alongside the Clinical Research Network East of England (CRN EoE), which does a fantastic job to supporting the delivery of research. Have a look at Our local strategy which was published just a couple of months ago.
There are four core principles, and we are now in the process of producing an implementation plan:
- Focused on our communities
- Driven by a confident and capable workforce
- Collaborative and coordinated
- Embedded in everything we do as a system
As part of this I wanted to highlight Research Capability Funding (RCF). RCF is primarily used to support people (academics and clinicians) to develop and submit competitive applications for research funding to the National Institute of Health and Care Research (NIHR). Over the course of two rounds this year, we have funded 15 projects.
The difference in this year’s applications has been the strength of cross-system working and the involvement of the VCSE sector right at the start of developing grant proposals. We are really glad to see that our approach to the use of RCF is strengthening existing partnerships and bringing new organisations into research.
Awardees for the second round of RCF funding were notified on 9 October 2023, and here are a few examples of the amazing projects supported by RCF last year.
Norfolk County Council (NCC)
Development of an application to NIHR to evaluate a short-term autism support service and measuring its impact on autistic adults’ wellbeing. The aim of the service is to reduce longer term social care needs and enable people to live more independently. Collaboration between NCC, NHS Norfolk and Waveney ICB, Norfolk Community Health and Care NHS Trust and the Norfolk Autism Partnership Board has already undertaken a significant amount of co-design work. I think this really shows that research doesn’t have to always mean test tubes and lab work.
University of East Anglia
Development of an NIHR application to improve young carer support: optimising the Carer Support Needs Assessment Tool Intervention (CSNAT-I) for Young Carers. Focussed on young carers and how best to identify and support their needs. Partnership between multiple System partners and VCSE sector, particularly Great Yarmouth and Gorleston Young Carers.
Development of an NIHR application to improve the acceptability of collecting meaningful outcome measures with people from under-researched groups. The team are working with three community organisations: A women’s organisation in Great Yarmouth, a community organisation in Norwich and an organisation supporting asylum seekers and refugees, to think about and capture what matters to people when they are taking part in research. The aim of the larger grant is to co-produce a set of outcome measures that are meaningful to people and communities that are beyond regular clinical or quality of life measures. Like the NCC project, this one is another brilliant demonstration of how we want to use research to have an immediate impact on the lives of our citizens, in this case specifically to help support young carers.
University of Suffolk (UoS)
Development of an application to assess embedding an integrated system approach to a Prehabilitation programme for cancer patients in Great Yarmouth and Waveney. Most cancer Prehabilitation programmes have been developed and embedded within acute organisations and have not included an integrated system approach to include Primary/ Social Care and Community organisations in their development or delivery. Colleagues at UoS, working with other providers and VCSE organisations. This one demonstrates how serious we are about acting early to improve health, in line with our Clinical strategy too.
So, I just wanted to highlight that we are really using our strategy: expanding who can be involved in research and the breadth of the research we want to support, to make sure that we undertake research that actually matters to our people. And to build on this further, we have just held a focused offer for Primary Care Networks (PCNs) – to try to build additional interest, capacity, and capability for research across our whole system. We’ve had a great response with applications demonstrating real enthusiasm and lots of new ideas which we’re looking forward to supporting this year to further increase our reach across our whole system.
Capital Projects
This is another amazing, good news story.
As you know, we have been campaigning for new hospitals to replace the Queen Elizabeth Hospital King’s Lynn NHS Foundation Trust (QEH) and the James Paget University Hospitals NHS Foundation Trust (JPUH) for many years and we have now finally been successful with both included on the New Hospital Programme. It is also great news that there is a national commitment to replace all RAAC plank hospitals across England by 2030, so the days of wards being decanted to temporary units while failsafe works take place, and the days of working around wooden posts and RSJs will soon be behind us.
This is obviously wonderful news, but we absolutely have to ensure that we don’t just replace the buildings with new versions of the old. The current plans have all been designed factoring in our current demand and capacity, as well as public health data on our changing and ageing demographic, and modelling against our joint strategic needs assessment. We are now pulling all of this together, as we are determined to use this as an opportunity to transform and really lever the best for our whole system out of this injection of capital.
So, there are three workstreams being led across the East of England region. A horizontal group looks at how the hospitals work together – for example if we build a “cold” or protected elective unit at one site, we might move activity from a second site there concentrating our resources, to improve the quality and the amount of operations we can perform. A vertical group looks at how the new hospitals should be used as part of a wider system, for example by exploring what services we want to provide through community hubs or virtually or at alternative sites. We need to make sure that we don’t design a huge new outpatient department if there will also be a community hub with clinic rooms in it nearby.
Finally, a productivity group is in place to make sure that the new hospital programme ensures value for money, both in their own design and for the region. We are also following national programme advice for example, have single bedded rooms to improve infection, prevention and control, and improve efficiency by reducing the need for non-clinical moves; and other no brainers like designing and building in decent Wi-Fi coverage and cabling to support new ways of working from the start.
So, we are now pulling all of these together within our system, and are reviewing the current schemes together, not just with the JPUH and QEH teams but with our other system partners and tying it to our ICS clinical strategy.
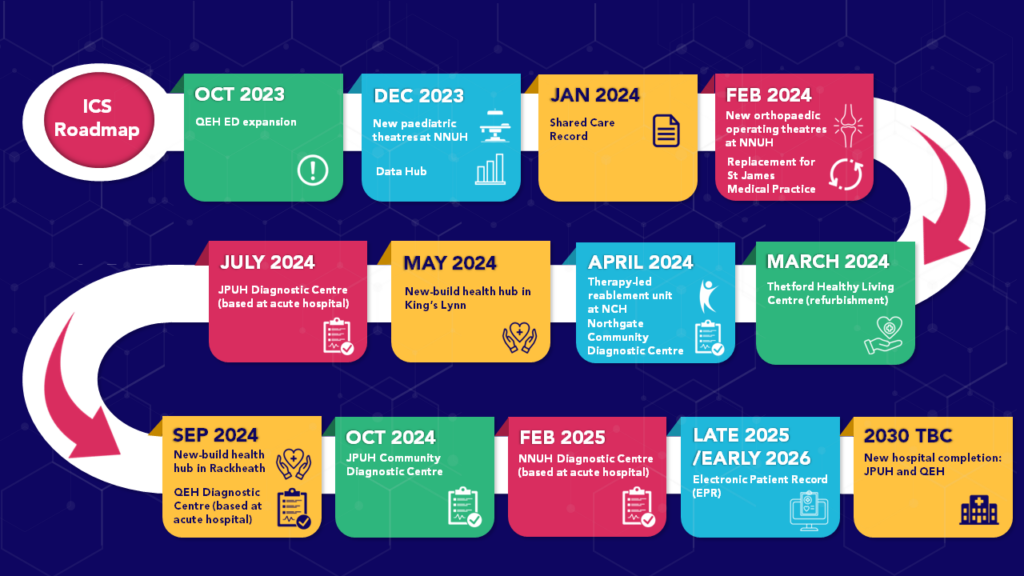
But, it’s not just about the new hospital programme. I was at QEH last week to look round the new section of their emergency department which is due to open 23 October.
New paediatric operating theatres are due to open at NNUH in December, with the state of the art orthopaedic centre (NANOC) soon to follow in January 2024, and there are some brilliant projects underway in our community too – from health hubs to diagnostic centres, primary care estates upgrades to the new therapy led enablement unit.
Clinical and Care Professional Leadership (CCPL) manifesto update
You’ll hopefully remember the work we’ve done to create and deliver against a CCP manifesto which was published last year. We have made good progress with this and essentially delivered on six of the 10 pledges. We are about to send out our second annual survey to take the temperature of all of our CCPL leaders to see how well this is working.
One key area that we have been working on recently is the short, medium and long term organisational development and education plan, rolling educational events and extending the reach of our CCPL community.
Leadership development support is now available for all of our CCPL workforce. Andy Griffiths, my deputy Medical Director has started and is leading this work and building a community of practice – bringing our Primary care network clinical directors, specialty advisors and locality leads together, as well as building a much broader CCPL faculty.
We have just launched a number of different programmes of support so we hope that there will be something suitable for all, whatever your background or development need.
Complex conversations
If you wish to nominate someone the sign-up is at this link. I am happy for it to be open equally to CCPL and non-CCPL leaders and managers.
Leadership Lunch and Learn sessions.
A series of 6 one-hour sessions facilitated by John Sutherland, a respected leader, author and academic who will share his take on aspects of leadership and culture; unpacking culture through a focus on four drivers of behaviour; Trust, Decision Making, Communication and Incentives and closing with a session on reflective and command leadership. These sessions are open to anyone within the ICS and form part of an Incubator offer for those new to leadership. You can sign-up at this link.
Sign-up to the Clinical and Care Professional Leadership Faculty.
We have also set up a faculty for aspiring system leaders within the ICS. It is open to anyone across the Norfolk and Waveney system and will allow us to keep in touch with you about future leadership offers and opportunities across the ICS. You can sign up for the faculty using the same link as above but instead simply decline the invitation for the lunch and learn sessions.
A Propagator offer to support potentially appointable leaders, an equaliser offer is specifically designed to support potential leaders who may not have had as many advantages and opportunities in the past, and the Consolidator programme for established leaders are all currently in development and will be launched soon. More details will follow shortly.
Finally, I just wanted to say a big thank you to everyone across our Integrated Care System for all your hard work and support over the last few months particularly. It has and continues to be an extremely busy and demanding time – your hard work and tenacity does not go unrecognised.
I’d also like to extend this message of thanks to our residents and communities for your patience and understanding at what remains the busiest and most demanding time for health and care services across Norfolk and Waveney and indeed the rest of the country.
